Dermatology Spotlight
Obesity is a multi-organ disease that affects the entire human organism. The skin is no exception; skin changes in people living with obesity have been widely studied, with 60% to 70% of patients with obesity presenting with a variety of skin changes. Metabolic syndrome and obesity are often responsible for the epidemiological prevalence of skin inflammation and are involved in the pathogenesis of chronic inflammatory skin diseases, such as psoriasis, atopic dermatitis, and skin malignancies.1,2
Physiologically, obesity contributes to a range of skin conditions through mechanical stress, metabolic dysregulation, and immune system alterations, with evidence increasingly supported by dermatologic and nutritional research. Obesity alters skin physiology in ways that predispose individuals to dermatologic disorders. For example, excess adipose tissue increases skin folds and friction, leading to conditions such as intertrigo, candidiasis, and folliculitis. These mechanical effects are compounded by impaired skin barrier function, which is influenced by systemic inflammation and metabolic changes. Data have shown that obesity is also associated with increased transepidermal water loss and reduced stratum corneum hydration, both of which compromise the skin’s protective capacity and healing potential.3
Metabolic dysfunction in obesity also contributes to specific skin manifestations. Acanthosis nigricans, characterized by hyperpigmented, velvety plaques in intertriginous areas, is strongly linked to insulin resistance. Skin tags (acrochordons) are more prevalent in obese individuals and may reflect underlying metabolic syndrome. Obesity-related malnutrition—particularly deficiencies in micronutrients like zinc and vitamin D—can impair skin integrity and immune responses, exacerbating conditions such as psoriasis and atopic dermatitis.4
Addressing obesity is essential for improving skin health. Dietary interventions, including increased intake of prebiotics, probiotics, and essential fatty acids, have shown promise in restoring skin barrier function and reducing inflammation.3 Weight reduction with weight loss medications such as GLP-1/GIP receptor agonists not only alleviates mechanical stress but also improves metabolic parameters, which can lead to resolution or improvement of obesity-associated skin conditions. A multidisciplinary approach that includes dermatologic care, nutritional support, lifestyle modification, and medication is important for managing these complex interactions between obesity and skin health.
References
- Darlenski R, et al. Front Nutr. 2022;9:855573.
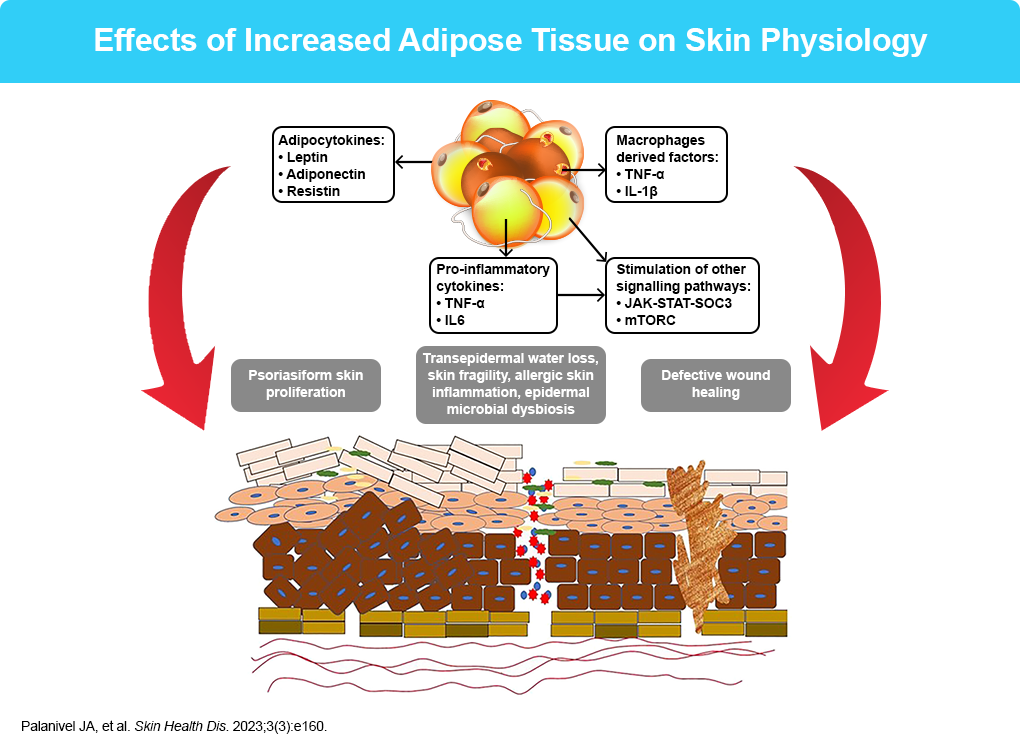
- Palanivel JA, Millington GWM. Skin Health Dis. 2023;3:e160.
- Parke MA, et al. Dermatol Pract Concept. 2021;11:e2021132.
- Cristancho C, et al. Nutr Clin Pract. 2024;39:1300-1316.