Patient Support Strategies
Supporting patients with obesity and inflammation requires a multifaceted approach that integrates behavioral, nutritional, and physiological strategies to reduce systemic inflammation and improve long-term outcomes.
Behavioral interventions are foundational to patient support, particularly those that enhance motivation and self-efficacy. Techniques like motivational interviewing and cognitive behavioral therapy (CBT) have shown efficacy in promoting sustainable lifestyle changes and reducing inflammatory markers. CBT, for example, helps patients identify maladaptive eating patterns and emotional triggers, which are often linked to chronic inflammation and metabolic dysfunction.1 Additionally, sleep hygiene and circadian rhythm alignment are emerging as critical components of behavioral support, as disruptions in sleep/wake cycles can exacerbate adipose tissue inflammation and insulin resistance.2
Nutritional counseling plays a central role in managing inflammation in obese patients. Diets rich in anti-inflammatory components—such as omega-3 fatty acids, fiber, and polyphenols—can reduce levels of TNF-α, IL-6, and CRP. The Mediterranean diet, in particular, has demonstrated benefits in lowering systemic inflammation and improving metabolic profiles.3 Personalized nutrition plans that consider metabolic phenotype and inflammatory biomarkers are more effective than generic advice, especially when combined with microbiome-targeted strategies like prebiotics and probiotics. These interventions help restore gut barrier integrity and reduce endotoxin-driven inflammation.4
Multidisciplinary care and obesity counseling are essential for sustained support.5 Coordinated teams involving primary care providers, specialists, dieticians, psychologists, physical therapists and others can address the complex interplay between obesity, inflammation, and comorbid conditions. For example, integrating circadian biology into care plans—such as aligning meal timing and physical activity with biological rhythms—may enhance metabolic adaptation and reduce adipose tissue inflammation.3 Digital health tools, including mobile apps and telehealth platforms, further empower patients by facilitating self-monitoring and real-time feedback. Together, these strategies foster long-term engagement and improve both inflammatory and metabolic outcomes.
References
- Yearwood L, Masood W. Behavioral Approaches to Obesity Treatment. [updated 1/31/2024 ]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025.
- Kiehn JT, et al. Compr Physiol. 2017;7:383-427.
- Scheiber A, Mank V. Anti-Inflammatory Diets. [updated 10/28/2023]. In: StatPearls [Internet].Treasure Island (FL): StatPearls Publishing; 2025.
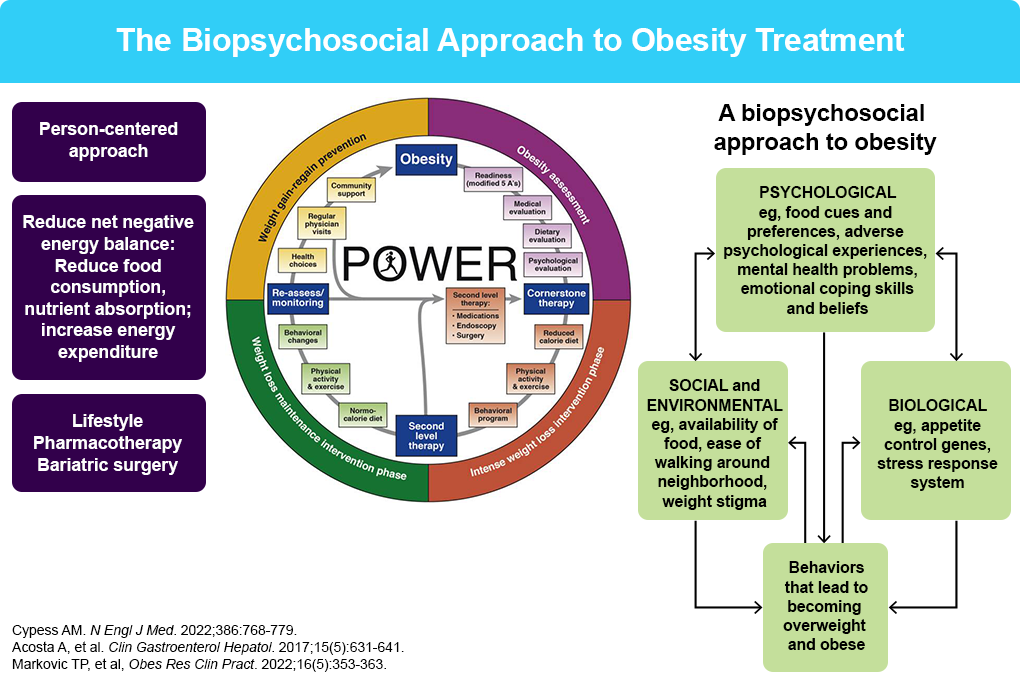
- Cypess AM. N Engl J Med. 2022;386:768-779.
- Acosta A, et al. Clin Gastroenterol Hepatol. 2017;15:631-649.
- Markovic TP, et al. Obes Res Clin Pract. 2022;16:353-363.
- Elmaleh-Sachs A, et al. JAMA. 2023;330:2000-2015.